Introduction
Gastrectomy is the removal of part or all the stomach. Removing your stomach doesn’t take away your ability to digest liquids and foods but the patient often needs to change some eating styles.
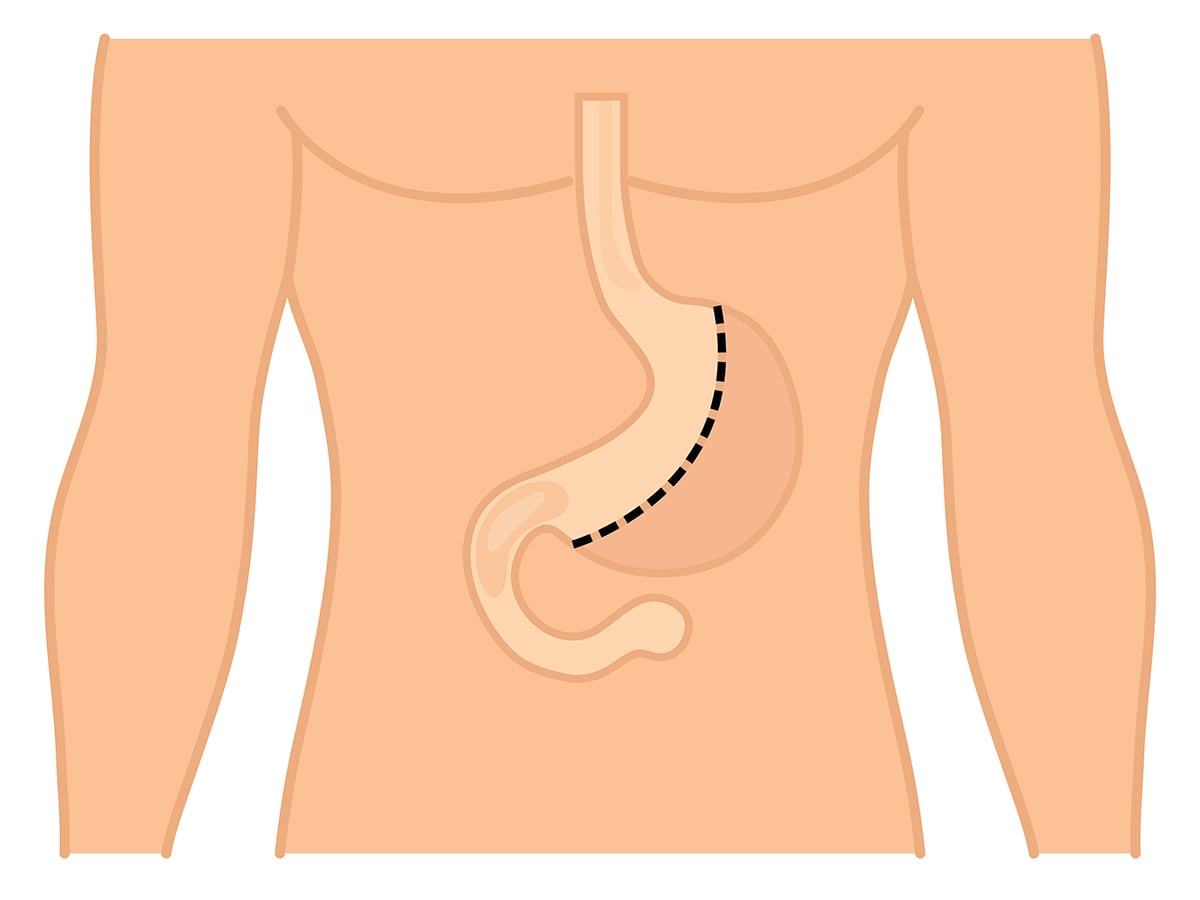
Partial Gastrectomy
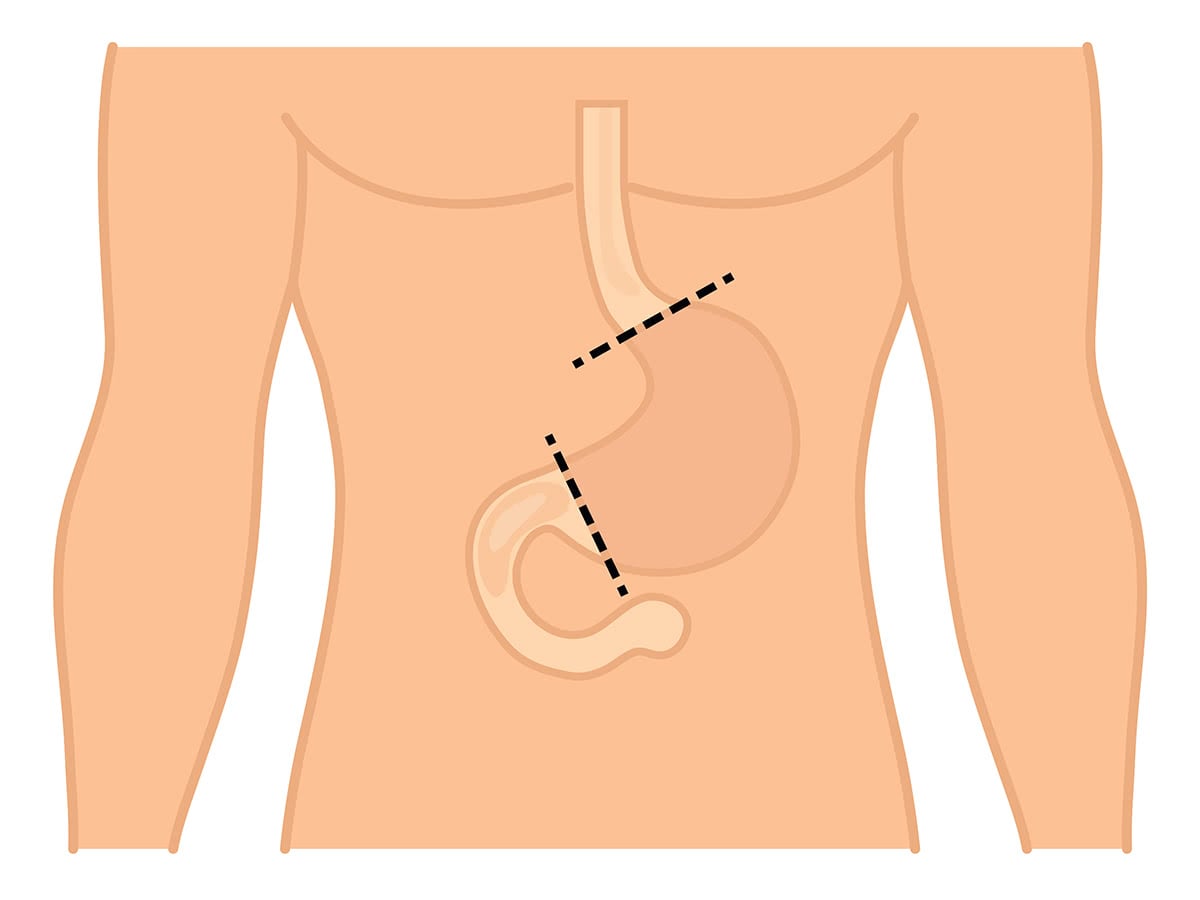
Total Gastrectomy
There are three main types of gastrectomy:
Partial gastrectomy
This is the removal of a part of the stomach. A distal gastrectomy is when the lower half is removed.
Total Gastrectomy
This is the removal of the entire stomach.
Subtotal gastrectomy
This is when most of the stomach is removed except the upperpart.
Indications
Your doctor may recommend a gastrectomy to treat:
- Benign, or noncancerous, tumours.
- Bleeding.
- Inflammation.
- Perforations in the stomach wall.
- Polyps, or growths inside your stomach.
- Stomach cancer.
- Severe peptic or duodenal ulcers.
Types of Gastrectomy
Distal Gastrectomy
Distal gastrectomy involves removing the lower portion of the stomach (generally one half) until a good clearance from the tumour is achieved. This operation would also involve taking out the lymph nodes adjacent to the tumour.
The second part of the operation is joining the remained stomach to the jejunum to restore the continuity.
Subtotal Gastrectomy
Same as distal except that most of the stomach is removed and the remaining upper part is connected to the bowel.
Total Gastrectomy
This procedure completely removes the stomach. Your surgeon will connect your oesophagus directly to your small intestine. The oesophagus normally connects your throat to your stomach.
Approach to the above operations
There are two different ways to perform gastrectomy no matter what the type was. All are performed under general anaesthesia. This means you’ll be in a deep sleep during the operation and you won’t be able to feel any pain.
Open surgery
Open surgery involves a single, large incision. Your surgeon will pull back skin, muscle, and tissue to access your stomach.
Laparoscopic surgery
Laparoscopic surgery is minimally invasive surgery. It involves small incisions and specialized tools. This procedure is less painful and allows for a quicker recovery time. It’s also known as “keyhole surgery”. It’s a more advanced surgery with a lower rate of complications.
Risks
The risks of a gastrectomy include:
- Infective complications.
- Leaking from the stomach at the operation site.
- Nausea or vomiting which may indicate delayed gastric emptying,
- Bleeding.
- Stomach acid leaking into your oesophagus, which causes scarring, narrowing, or constriction (stricture).
- A blockage of the small bowel.
- Vitamin deficiency.
- Weight loss.
Postoperative Instructions
- You can expect to stay in the hospital for one to two weeks after the surgery. During this period, you’ll likely have a tube running from your nose to your stomach. This allows your doctor to remove any fluids produced by your stomach. This helps keep you from feeling nauseated.
- You may be fed through a tube in your vein until you’re ready to eat and drink normally.
- Tell your doctor immediately if you develop any new symptoms or pain that’s not controlled with medication.
Lifestyle changes
Once you go home, you may have to adjust your eating habits. Some changes may include:
- Eating smaller meals throughout the day.
- Avoiding high fibre foods.
- Eating foods rich in calcium, iron, and vitamins C and D.
- Taking vitamin supplements.
Eating small meals and snacks are more tolerated. Then, you’ll be able to consume more fibre and eat larger meals. You’ll need to have regular blood tests after the procedure to make sure that you’re getting enough vitamins and minerals.